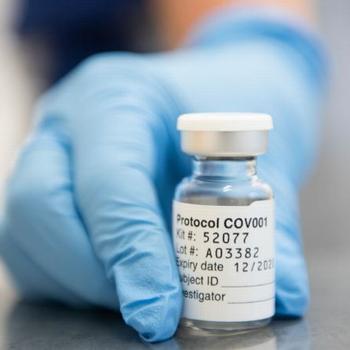
LONDON, UK, January 4, 2021 (ENS) – The first vaccinations using the Oxford University/AstraZeneca coronavirus vaccine were given today to members of the British public as the National Health Service expands COVID-19 vaccination programs across the UK.
It turns out that the vaccine rollout came on the same day that Prime Minister Boris Johnson issued an urgent order for a six-week lockdown in an attempt to curb the soaring infection rate. To date, the UK has reported 2,713,563 cases and 75,431 deaths across the country.
The Prime Minister, who himself recovered from a bout of the virus last year, ordered, “You must stay at home. The single most important action we can all take is to stay at home to protect the NHS [National Health Service] and save lives. You should follow this guidance immediately. The law will be updated to reflect these new rules.”
For the next six weeks, the public may leave the home only to shop for necessities, go to work, exercise in their local area, seek medical help and attend education or child care if authorized.
But at 7.30 am, when dialysis patient Brian Pinker at the Oxford University NHS Hospitals Trust became the first person to be vaccinated as part of the UK’s rollout of the Oxford/AstraZeneca coronavirus vaccine, Prime Minister Johnson had not yet given the order, and the mood was upbeat. Everyone was hopeful that the long coronavirus ordeal might finally come to an end.
Health Secretary Matt Hancock said, “I am delighted that today we are rolling out the Oxford vaccine – a testament to British science. This is a pivotal moment in our fight against this awful virus and I hope it provides renewed hope to everybody that the end of this pandemic is in sight.”

The NHS is the first health service in the world to deploy this vaccine, which has been authorized by the Medicines and Healthcare products Regulatory Agency, MHRA, after meeting strict standards of safety, quality and effectiveness. It is the only approved vaccine that can be stored at regular refrigerator temperatures.
More than a million people in the UK have already been vaccinated with the Pfizer/BioNTech vaccine and its rollout will continue at pace. And now there is a second vaccine available for UK residents.
The government has secured access to 100 million doses of the Oxford University/AstraZeneca vaccine on behalf of the whole of the UK, crown dependencies and overseas territories.
More than half a million doses are available today, with tens of millions more to be delivered in the coming weeks and months once batches have been quality checked by the MHRA.
More than 730 vaccination sites have already been established across the UK and hundreds more are opening this week to take the total to over 1,000, helping those who are most at risk from COVID-19 to access vaccines for free, regardless of where they live.
“Through its vaccine delivery plan the NHS is doing everything it can to vaccinate those most at risk as quickly as possible and we will rapidly accelerate our vaccination program,” Hancock said.
“While the most vulnerable are immunized, I urge everybody to continue following the restrictions so we can keep cases down and protect our loved ones,” Secretary Hancock said.
The first Oxford/AstraZeneca vaccinations will be delivered at hospitals for the first few days, as is standard practice before the bulk of supplies are sent to hundreds of doctor-led services and care homes later in the week.
Because the Oxford/AstraZeneca vaccine can be stored at regular fridge temperatures, between two to eight degrees Celsius, it is easier to distribute to care homes and other locations across the UK than the Pfizer/BioNTech vaccine which must be stored at temperatures between -80°C and -60°C.

ChAdOx1 nCoV-19, now known as AZD1222 co-invented by the University of Oxford and its spin-off company, Vaccitech, is being trialed by the University’s Jenner Institute and Oxford Vaccine Group. The team started working to develop a vaccine against coronavirus in January 2020.
Developed at the Jenner Institute, the recombinant adenovirus vector ChAdOx1 nCoV-19 uses a viral vector based on a weakened version of the common cold virus (adenovirus) containing the genetic material of SARS-CoV-2 spike protein.
After vaccination, the surface spike protein is produced, which primes the immune system to attack COVID-19 if it later infects the body.
Vaccines made from the ChAdOx1 nCoV-19 virus have been given to around 11,000 people to date and have been shown to be safe and well-tolerated, although they can cause temporary side effects, such as a temperature, flu-like symptoms, headache or sore arm.
The potential vaccine entered Phase III clinical trials in May to study safety and efficacy in healthy volunteers aged 18 to 55 years, across 19 trial sites in the UK. The University of Oxford is also working with research partners at a number of clinical trial sites around the world as part of this late-stage trial.
In line with the recommendations of the UK Joint Committee on Vaccination and Immunisation, the vaccine will be rolled out to the priority groups – care home residents and staff, people over 80 and health and care workers – then to the rest of the population in order of age and risk, including those who are clinically extremely vulnerable.
General practitioners and local vaccination services have been asked to ensure every care home resident in their local area is vaccinated by the end of January.
The COVID-19 vaccines will be deployed through:
* – hospital hubs for NHS and care staff and older patients
* – local community services with local teams and general practitioners already signing up to take part in the program
* – vaccination centers across the country, ensuring people can access a vaccine regardless of where they live
An army of current and former NHS staff have applied to become vaccinators, with tens of thousands having already completed their online training. They are being processed as quickly as possible and volunteer vaccinators will be deployed as more vaccine supplies become available.
The MHRA, Joint Committee on Vaccination and Immunisation and the four UK chief medical officers agreed to delay the gap between the first and second dose of vaccines to protect the greatest number of people in the shortest amount of time.
Copyright Environment News Service (ENS) 2021. All rights reserved.
© 2021, Environment News Service. All rights reserved. Content may be quoted only with proper attribution and a direct link to the original article. Full reproduction is prohibited.



