BOSTON, Massachusetts, July 2, 2021 (ENS) – Scientists have found a way to embed synthetic biology-based sensors into fabrics, creating wearable biosensors that can be programmed to detect pathogens and toxins and to alert the wearer via a companion smartphone app.
The team from the Wyss Institute for Biologically Inspired Engineering at Harvard University and the Massachusetts Institute of Technology has integrated this technology into standard face masks to detect the presence of the SARS-CoV-2 virus in a patient’s breath.
The button-activated mask gives results within 90 minutes at levels of accuracy comparable to standard nucleic acid-based diagnostic tests like polymerase chain reactions, known informally as PCR. The achievement is reported in the June 28 issue of the journal “Nature Biotechnology.”
“We have essentially shrunk an entire diagnostic laboratory down into a small, synthetic biology-based sensor that works with any face mask, and combines the high accuracy of PCR tests with the speed and low cost of antigen tests,” said co-first author Peter Nguyen, PhD, a research scientist at the Wyss Institute.
“In addition to face masks,” Dr. Nguyen said, “our programmable biosensors can be integrated into other garments to provide on-the-go detection of dangerous substances including viruses, bacteria, toxins, and chemical agents.”
The technique involves extracting and freeze-drying the molecular machinery that cells use to read DNA and produce RNA and proteins. These biological elements are shelf-stable for long periods of time and activating them is simple: just add water.
Synthetic genetic circuits can be added to create biosensors that can produce a detectable signal in response to the presence of a target molecule.
“This technology could be incorporated into lab coats for scientists working with hazardous materials or pathogens, scrubs for doctors and nurses, or the uniforms of first responders and military personnel who could be exposed to dangerous pathogens or toxins, such as nerve gas,” said co-author Nina Donghia, a staff scientist at the Wyss Institute.
The researchers first applied this technology to diagnostics by integrating it into a tool to address the Zika virus outbreak in 2015. They created biosensors that can detect pathogen-derived RNA molecules and coupled them with a colored or fluorescent indicator protein, then embedded the genetic circuit into paper to create a cheap, accurate, portable diagnostic.
Following their success embedding their biosensors into paper, the team of scientists next set their sights on making them wearable.
“Other groups have created wearables that can sense biomolecules, but those techniques have all required putting living cells into the wearable itself, as if the user were wearing a tiny aquarium. If that aquarium ever broke, then the engineered bugs could leak out onto the wearer, and nobody likes that idea,” said Dr. Nguyen.
He and his teammates started investigating whether their technology could solve this problem, testing it in more than 100 different kinds of fabrics.
The SARS-CoV-2 biosensor is the culmination of three years of work on what the team calls their wearable freeze-dried cell-free, wFDCF, technology, which is built upon earlier versions created in the lab of Wyss Core Faculty member and senior author Jim Collins, PhD, a professor of medical engineering and science at MIT.
Then, the COVID-19 pandemic struck and the scientific team pivoted from wearables in general to focus on face masks.
“We wanted to contribute to the global effort to fight the virus, and we came up with the idea of integrating wFDCF into face masks to detect SARS-CoV-2,” said co-first author Luis Soenksen, PhD, a postdoctoral fellow at the Wyss Institute.
The entire project was done under quarantine or strict social distancing starting in May 2020.
“We worked hard, sometimes bringing non-biological equipment home and assembling devices manually,” Soenksen said. “It was definitely different from the usual lab infrastructure we’re used to working under, but everything we did has helped us ensure that the sensors would work in real-world pandemic conditions.”
How These Face Masks Work
The final product consists of three different freeze-dried biological reactions that are sequentially activated by the release of water from a reservoir with the single push of a button.

When SARS-CoV-2 particles are present, the wFDCF system cuts a molecular bond that changes the pattern of lines that form in the readout strip, similar to an at-home pregnancy test.
The first reaction cuts open the SARS-CoV-2 virus’ membrane to expose its RNA. The second reaction is an amplification step that makes numerous double-stranded copies of the Spike-coding gene from the viral RNA. The final reaction uses CRISPR-based SHERLOCK technology to detect any Spike gene fragments, and in response cut a probe molecule into two smaller pieces that are then reported via a lateral flow assay strip.
Whether or not there are any Spike fragments available to cut depends on whether the patient has SARS-CoV-2 in their breath.
This is reflected in changes in a simple pattern of lines that appears on the readout portion of the device, similar to an at-home pregnancy test.
The wFDCF face mask is the first SARS-CoV-2 nucleic acid test that achieves high accuracy rates comparable to current gold standard RT-PCR tests while operating fully at room temperature, eliminating the need for heating or cooling instruments and allowing the rapid screening of patient samples outside of labs.
“This work shows that our freeze-dried, cell-free synthetic biology technology can be extended to wearables and harnessed for novel diagnostic applications, including the development of a face mask diagnostic.
Dr. Collins said, “I am particularly proud of how our team came together during the pandemic to create deployable solutions for addressing some of the world’s testing challenges.”
Now, the team is actively searching for manufacturing partners who are interested in helping to enable the mass production of the face mask diagnostic for use during the COVID-19 pandemic, as well as for detecting other biological and environmental hazards.
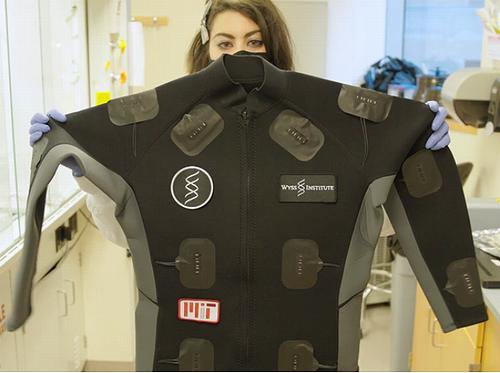
Featured image: The Wyss Institute’s wearable freeze-dried cell-free (wFDCF) technology can quickly diagnose COVID-19 from virus in patients’ breath, and can be integrated into clothing to detect a wide variety of pathogens and other dangerous substances. 2021 (Photo courtesy Wyss Institute at Harvard University)
© 2021, Environment News Service. All rights reserved. Content may be quoted only with proper attribution and a direct link to the original article. Full reproduction is prohibited.